Date: Sat, 5 Jan 2002 11:27:49 +0500
Subject: Pseudarthrosis of the femoral neck
Hello all,
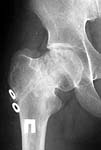
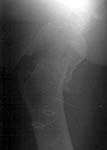
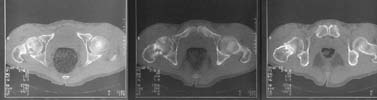
A male (32 y.o, 175 cm, 65 kg) after a car accident 1 year ago sustained a femoral neck fracture. The fracture was fixed elsewhere by cancellous screws. He noted telescoping of the screws four month later. Recently the screws have been removed. Walks with cane and marks hip pain. Xrays and CT (see attachment) demonstrate pseudarthrosis of the neck.
 |
 |
 |
Osteotomy looks more preferable in the rather young patient. What sort of osteotomy is optimal for the pattern?
Or i am wrong and THA is a primary choice here? What additional data would help to make a decision?
THX in advance.
Best regards,
Alexander N. Chelnokov
Ural Scientific Institute of Traumatology and Orthopaedics
str.Bankovsky, 7. Ekaterinburg 620014 Russia
Date: Sat, 05 Jan 2002 00:06:30 -0700
From: seannork
Hello Alex
In a 32 year old male with a femoral neck nonunion, his best option is probably a valgus producing intertrochanteric osteotomy with blade plate fixation. In the preoperative planning stage, neutral rotation (patella up) 100% films of both hips are necessary. The AP film enclosed is with significant external rotation given the appearance of the lesser trochanter. It doesn't appear that there is significant retroversion based on the CT scan. Depending upon what his neck shaft angle is compared with his normal side, a better recommendation of the degree of osteotomy can be made. Predictable results (ie union) can be obtained without trying to reproduce a fracture angle of 25 degrees. That is, a 20 or 30 degree valgus producing intertrochanteric osteotomy with a 110 degree or 120 degree blade plate, respectively, should give a reliable result. According to the preoperartive plan with comparison to the contralateral hip in the same rotation, the lateralization of the shaft can be accomplished to help minimize proximal deformity and lateral compartment overload of the knee (theoretically). Length can be simultaneously gained as well.
I'm sure the next question is whether any other studies should be done to investigate further the vascular supply to the head. I would argue that, in a 32 year old, vascular compromise is not a contraindication to an intertrochanteric osteotomy and MRI/other tests are not necessary (see Marti, R; JBJS [Br], mid 80's). The head will frequently revascularize after union. The alternatives are limited as well.
Good luck.
Sean Nork, MD
HMC, Seattle
Date: Sat, 05 Jan 2002 00:08:30
From: Bill Burman
Alex
Two previous femoral neck nonunion cases presented to the OTA Case Discussion Forum which may be worth reviewing:
Date: Sun, 06 Jan 2002 09:54:57 -0600
From: Adam Starr
I agree about the vascular status of the head. I think I would try to salvage this one, even if I knew that the blood supply was damaged. At least, if I was this guy, I'd want to try to keep my own bone. 32 is awful young for a total hip.
The people who swear by vascularized fibula grafts would (maybe) say that the use of that technique would increase the chance of head survival and fracture union...but I have no experience with vascularized fibula grafts.
Adam Starr
Dallas
Date: Mon, 07 Jan 2002 09:08:34 -0600
From: Steven Rabin
Most 32 year olds should be treated with osteotomy. However, I am concerned that the x-rays imply some early avascular necrosis (there is some lucency and irregularity in the superior femoral head), and I would at least obtain an MRI to assess its extent if it is present. This can give an idea as to prognosis. If AVN is present, I would consider adding either a vascularized fibula to my osteotomy procedure or a vascularized quadratus femoris bone block transfer to try to increase the chance of healing. If there is extensive whole head involvement of AVN, then I might even consider hip replacement even at this age (although I'd again prefer to do osteotomy), because hip replacement after osteotomy with the deformed femoral canal can be much more technically difficult and if failure appears inevitable, why make the next surgery harder? Again, first choice is osteotomy, but I'd like to know the femoral head's status before surgery. (In the litiginous USA, it might also be useful to know that the AVN was present before the osteotomy so that when it develops postop, the osteotomy surgery isn't blamed.)
Finally, I also search for infection as a cause of nonunion when a patient has had previous surgery, so I would also obtain a complete blood count including white blood cell count, differential, and sedimentation rate preop.
good luck
steve rabin
loyola