Date: Sun, 16 Mar 2003 14:05:07 -0500
Subject: Open ankle fracture with syndesmosis disruption
Dear participants,
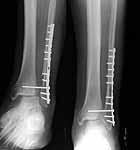
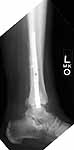
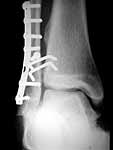
Below is a case referred to me by a fellow orthopaedic surgeon. This is a 50 y.o. gentleman s/p motorcycle accident who suffered an open ankle fracture with syndesmosis disruption. The open wound was over the medial malleolus. He was treated with I&D and ORIF. Postop xrays revealed disruption of the ankle mortise and he was taken back to the OR where a tibiotalar pin was placed after reduction of the ankle mortise. The pin was removed a few weeks later and his ankle subluxed again. He was then referred to me.
He is currently approximately 4 months out from the injury. He has no overt signs of infection and his ESR and CRP are normal. His fibula appears out to length but I believe is malrotated and his syndesmosis is malreduced. I plan to remove hardware, obtain cultures and reduce the syndesmosis and hold it with two syndesmotic screws. I also plan to open the medial side and remove any scar tissue in the ankle joint preventing reduction. I appreciate any other comments.
 |
 |
Nicholas Divaris, MD
SUNY Stony Brook University Hospital
Date: Sun, 16 Mar 2003 16:29:56 -0500
From: Clifford Jones, M.D.
The fibula is short. You must osteotomize to lengthen fibula. Open medially and debride. Open distal syndesmosis to perform anatomic lengthening and reduction. CT pre op may help to evaluate distal syndesmosis, i.e. post or ant malreduction. Final reduction with 2 hole 1/3 tubular and 2 x 3.5 mm 4 cortices cortical screws. NWB x 6 wks, supported WB x an additional 6 wks. Do not remove syndesmosis screws unless necessary.
C Jones
Date: Sun, 16 Mar 2003 20:56:52 EST
From: Tadabq
Regarding case of unreduced syndesmosis (syndesmosis screw) with distal fibula (plated), posterior lip distal tibia and open deltoid ligament disruptions, 4 months from injury. Ops x2 or 3.
If you leave it, the prognosis is poor.
A CT scan would help assess the actual size of the posterior lip fracture.
You can perhaps improve the prognosis with corrective fibular osteotomy, reduction of fibula, clean out the medial space, reduce the syndesmosis and stabilize it. The posterior lip could also be reduced and fixed. Although not "usually" necessary, in a tough situation like this reduction and fixation of the posterior lip can be quite helpful.
You mentioned removal of hardware and reduction of the syndesmosis with placement of 2 syndesmosis screws. How do you plan to reduce the syndesmosis? If you try to squeeze it together without performing an osteotomy of the fibula it is likely to spring apart later or never reduce and you are on the way to a staged ankle fusion. Weber has a nice description of fibular osteotomy for malreduction circa 1985.
Has the syndesmosis ever been reduced? I don't think so. The fibula looks malreduced to me. From the pin tracks in the tibia and talus it looks like the medial clear space has always been wide. Is there something in it like posterior tibial tendon? Keep that in mind when you are "debriding" it.
Good luck.
TD
Date: Sun, 16 Mar 2003 21:19:40 -0600
From: Frederic B. Wilson, M.D.
What strikes me about this particular malunion is the tendency to treat ankle fractures as though all they need is a plate and a squeeze with the application of a syndesmosis screw or two. As was so elegantly shown by Paul Tornetta, however, we are coming to find out that none of that matters as much as achieving an anatomic reduction of the fibula with respect to it's length, rotation, and reduction in the fibular groove along the lateral distal tibia. In his paper presented at the AAOS and OTA, fixation with ONLY syndesmosis screws led to predictably good to excellent results.
In trying tosalvage this ankle it would seem that removing the plate and then performing an osteotomy (or even carefully taking down the fracture site) might allow pulling the distal fragment out to length and verifyingreduction by comparison to radiographs of the contralateral ankle. Carefully cleaning out the syndesmosis may mitigate the necessity of trying to"read" this old fracture which has been malreduced, and allow carefully placing it in the proper length, rotation, and position in the groove. The presence of soft tissue in the medial clear space (e.g. deltoid ligament) should be considered but is not likely the reason for the malreduction here. I've only had one or two instances where I wasn't able to close down the mortise without opening the medial side, although there are still some who would advocate a formal repair of the deltoid.At this late date I am not sure that would be a satisfying endeavor.
Bon chance.
Fred
Frederic B. Wilson, M.D.
Assistant Professor Trauma and Adult Reconstruction
Department of Orthopaedic Surgery Tulane University School of Medicine
New Orleans, Louisiana
Date: Sun, 16 Mar 2003 19:45:31 -0800
From: Robert W Chandler
There may be soft tissue in the syndesmosis. Measure the talocrural angle tocalculate the amount of fibular shortening present, therefore the amount of lengthening needed. You need comparison films of the opposite side to do so. You may have to lengthen the fibula (use a 3.5 mm DCP not a 1/3 tubular), clear the tib-fib space and the medial clear space. It should not take much force to hold the tibial to the fibula, there is not suppposed to be anything in there. A femoral distractor may be of value in gaining length ( I have a scaled down version that uses 4.0mm ex fix pins).
Date: Sun, 16 Mar 2003 11:55 PM EST
From: Bill Burman
There have been a couple of cases lately where the fibular length has been called into question:
What is the best way to judge fibular length? The talocrural angle has been suggested but here
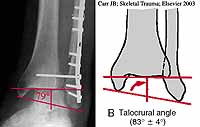 |
it is practically normal and has been reported by Michelson et al as unreliable.
Maybe a better guide is the medial fibular prominence which should be at the level of the joint line (see Ed Rutledge OTA BFC lecture).
In this case, the medial fibular prominence appears to be at the tip of 2nd to most distal fibular screw and above the joint line.
Date: Mon, 17 Mar 2003 00:30:20 -0600
From: John Early
I would tend to agree with the other respondents so far. the initial film shows a fibula about 1 cm short and that appears to be the major cause of the syndesmosis widening. there is usually some external rotation of the distal fracture also. On the Lateral film there appears to be some proximal displacement of the posterior lateral tubercle of the tibia. Ligaments between this and the fibula may hinder reduction and this fragment may need to be taken down and reduced also.
Through a lateral approach, remove the old hardware, recreate the fracture plane. I would also clean out the syndesmosis and free up the posterior tibial fragment. place an appropiate length plate, many will say a 3.5 dcp but a 1/3 tubular can also do the job, usually ~ 8 hole. Secure the plate slightly posterior lateral on the distal fragment for the last 3 holes. if an AO small plate distractor is not available, you can place a 3.5 mm screw through both fibular cortices just 0.5 cm above the proximal portion of the plate. using a laminar spreader, you can slowly displace the plate and attached distal fibula distal. This part is done slowly over a 10 minute period or so. You have to allow time for the soft tissue elasticity to provide for "stress relaxation". Usually as the fibula is advanced the distal fragment will rotate anteriorally and fall into its normal place. The proper length is the point at which the mortise is reduced. fix the plate to the proximal fibula, graft! the fibular gap and place a single syndesmosis screw.
Date: Mon, 17 Mar 2003 08:46:55 -0500
From: James Carr
I don't believe the fibula is short- it may be malrotated, or angled/displaced posteriorly. People forget that syndesmosis widening is a posterolateral rotatory instability of the talus+ some lateral fibular displacement. They see the lateral displacement, and get the urge to squeeze the tib-fib together (and then when it widens again, squeeze even harder!). The best way to tell is by direct exposure of the tibia-fibula articular junction. It will take some scar excision to expose this area. Normally you can see where they meet; the normal space between the tibia and fibula is ~ 1mm in plantar flexion, and ~3 mm (max) in dorsiflexion.
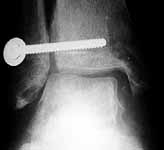
I would approach this problem by exposing medial, and reducing the talus to the medial side- hold it with a pin. I would then address lateral, and do whatever it took to reposition the fibula as others have stated so well. My personal preference for syndesmosis reconstruction is two medium barbed staples that parallel the ant tib-fib ligament (referenced in Kelikian's book on the ankle) +/- a ligament weave to try and reconstitute the tib-fib ligament. The staples stay in for good, and are more reliable than screws in my anecdotal experience. See attachments below. Patient presented after 3 attempts to squeeze the mortise down. Fibular shortening and malrotation present. Rx with lengthening and derotation + staple fixation of the syndesmosis.
 |
 |
James B. Carr, MD
Palmetto Health Orthopedics
Date: Tue, 18 Mar 2003 08:20:04 -0500
From: Fred Barrick
I believe that the cause of failure is either lack of reduction of the syndesmosis or, more likely, too weenie of a syndesmosis screw. I always use a 4.5 cortical screw, over drilling the fibula to get a lag effect. In this salvage stage, I think that reducing and fixing it will not hold. the concept initially is to reduce so that the stubby ends of the torn syndesmosis. I recommend a tibiofibular arthrodesis that includes a fibular osteotomy well above the ankle joint. Use bone graft and two screws to hold it. I have had two cases and both worked well. I will look up the references and post them later.
E. Frederick Barrick MD
Director of Orthopaedic Trauma
Inova Fairfax Hospital
Falls Church, VA 22042