Date: Mon, 26 Jan 2004 21:03:11 -0700
Subject: Comminuted Femoral Neck Fx
From: Terry Finlayson
To the List members
 |
 |
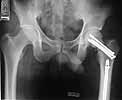
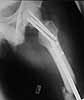
30 y/o man in head-on MVA 12/22/03 sustaining grade II open left femoral midshaft fracture (treated with appropriate staged debridement and retrograde statically locked IM nail), left lateral split tibial plateau fracture (treated with reduction and percutaneous cannulated screw fixation) and comminuted left femoral neck fracture (treated with open reduction and non-compression screw fixation). All initial treatment at another institution and patient recently came to me for follow-up care (he was travelling out of town when he was injured). He has a large (7cm) defect of lateral half of femoral shaft fracture which I plan to pack with a ton of bone graft next week (open fracture site soft tissues healed nicely without sign of infection).
What about the femoral neck? It's shortened, the head is inferiorly translated and I think probably in a little varus (hard to measure neck/shaft angle without a neck). However, I'm not sure I can improve the alignment given the significant bone loss, probable difficulty with repeat fixation once the current screws are removed and bone graft would almost certainly end up in the joint (no cortex to contain it). My inclination is to get the shaft to heal, try a bone stim on the neck and prepare bone stock for THA if/when neck doesn't heal, but I'm open to ideas from those more enlightened and/or optimistic than I am.
Thanks,
Terry I. Finlayson, M.D.
Alpine Orthopaedic Specialists
2380 N. 400 E. Suite A North Logan, UT 84341
Date: Tue, 27 Jan 2004 08:03:41 EST
From: Aobonedoc
Only small part of femoral shaft fracture visible on one xray. I would be interested in seeing xrays of the shaft fracture. I would be hesitant about bone grafting the femoral shaft fracture early. It might heal. Femoral neck fracture is going to be a problem. I agree, in varus and almost appears with some distraction at the fracture site. I do not think anything now will significantly increase the chance of salvage. I would suggest observation over a reasonable period of time while on crutches, documentation of healing or lack of healing with CT or tomogram (hard to get as the machines are fewer and fewer), then definitive treatment of what is left at the hip. Not an agressive approach but one that gives a 30 year old a chance to heal given how he was initially treated.
Sincerely and respectively,
M. Bryan Neal, MD
Date: Tue, 27 Jan 2004 11:43:11 -0700
From: Terry Finlayson
I didn't mean to imply that there was necessarily anything wrong with the way
he was initially treated; he had a bad injury and we all know you can't make
chicken salad out of chicken droppings. Will submit x-rays of femoral shaft
soon.
Terry Finlayson, M.D.
Date: Tue, 27 Jan 2004 16:19:52 -0800
From: Chip Routt
I agree that most femoral shaft fractures (even with defects) don't need
grafting, but without inclusive films it's difficult to make an opinion regarding
this shaft defect.
Speak to the initial surgeon. How did the shaft traumatic wound and local
defect appear? How much associated soft tissue injury? What interval did they use
for the femoral neck procedure? What did the surgeon tell you was found at
operation? How much bone was removed? What was the capsular condition within the
surgical interval? How did they handle that? Other surgical details? The neck is
currently malreduced, but what did the initial postop films show? Was it ever
reduced?
In a young active adult, very few would criticize you for a repeated attempt
at an accurate reduction and stable fixation. Assuming all answers to the above
questions are satisfactory, we'd strongly consider either repeat reduction and
fixation....or more likely proximal femoral
osteotomy for reorientation of the fracture line and blade plate fixation for
support. Reinhold Ganz once used the analogy of "supporting a rotten tomato with
strong, firm hands" for such a clinical scenario. Make some drawings and see what
they look like with osteotomy and blade fixation...you may be surprised.
You can't undo the event nor the previous procedure, but you can
improve/optimize the current fracture environment, which can have significant
impact on his outcome.
Share your decision-
Chip
M.L. Chip Routt, Jr.,M.D.
Date: Tue, 27 Jan 2004 19:42:54 -0700
From: Thomas Higgins
Terry
It looks like the films are one month into treatment. It is hard to think
that the hip will do well as it is. I also don't see how it is going to reduce
accurately anymore, as it appears some bone may be absent.
I don't know if you think a Pauwels-type valgus-producing osteotomy seems
overly aggressive, but it has much to offer. It would give you better alignment,
better length, and possibly a better likliehood of union. A blade would address
the fixation problem, and the operation does not burn bridges.
The issue of the shaft is harder to tell from the images, but could be
addressed concurrently or seperately, based on dedicated imaging.
Sincerely,
Thomas Higgins
Date: Wed, 28 Jan 2004 22:02:54 +0500
From: Alexander Chelnokov
Hello Terry,
TF> He has a large (7cm) defect of lateral half of femoral shaft
fracture which I plan to pack with a ton of bone graft next week
I agree with Bryan Neal that probably no need to hurry with this.
TF> What about the femoral neck? It's shortened, the head is
inferiorly translated and I think
Why not think about valgus osteotomy with blade plate?
The nail wouldn't prevent this.
Best regards,
Alexander N. Chelnokov
Date: Wed, 28 Jan 2004 14:38:13 -0500
From: Sam Agnew
Terry
I would preface my commentary with a complete agreement as to the comments
from Chip, regarding both the shaft and the neck dilemma.
>TF -- and comminuted left
femoral neck fracture (treated with open reduction and non-compression screw
fixation)
You mentioned that the initial procedure was percutaneous fixation of the
neck, one would assume from that information that no formal open exploration
was performed of the neck.
Therefore, the images sent seem to indicate bone loss from comminution,
correct?, and the alignment abnormality is from a rotational malposition of
the neck, as well as the impaction-comminution seen at the
basi-cervical-transcervical level.
I would strongly vote for revision ORIF-Watson
Jones approach, formal capsulotomy-reduction of the
malrotation-impaction-&-bonegrafting of the neck. It may require inferior neck
plating as described years ago by Professor Marti (Springer Verlag publishers).
With the present day added advantages of ortho-biologics (AGF/IgF aka Symphony,
these may hedge the bets as it were. Even if a prior open reduction was indeed
performed, my preference is still for the direct repair approach. Phil Kregor has
given some excellent talks on femoral fixation with great illustrations as well.
Good luck, and please share your thought process
Sam Agnew, M.D., FACS
Date: Thu, 29 Jan 2004 20:46:02 -0700
Reply-To: "Orthopaedic Trauma Association forum." List Members:
Thanks for input thus far.
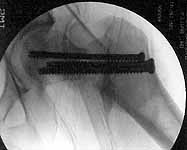
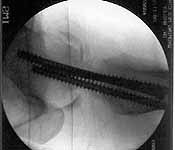
Some additional information. Initial neck treatment was open through lateral
incision with anterior exposure of the fracture. Op note mentions that intra-op
reduction of neck was suboptimal due to comminution, but makes no mention of
state of capsule and I haven't yet been able to speak directly with the treating
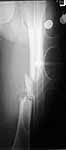
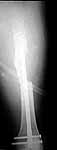
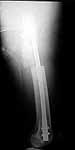
surgeon. Attached are intra-op films of neck and films of shaft (not great,
but show the cortical defect). Any further input is invited and welcome.
Terry Finlayson, M.D.
Date: Thu, 29 Jan 2004 23:00:27 EST
From: Aobonedoc
Hello:
I still would give this young patient 2-3 months from time of surgery to heal
and see what you are left with. Good luck. Please give (at least me, if you
do not mind), intermittent followup. Tough case.
Sincerely and respectively,
M. Bryan Neal, MD
Date: Fri, 30 Jan 2004 09:30:44 -0500
From: Sam Agnew, M.D.
Terry
Thanks for the added images, and information, I would again vote
wholeheartedly for doing something now, as opposed to waiting. Lateral
approache(s) to the femoral neck offer very limited exposure-visualization to the
entire neck , and thus probably the "suboptimal " reduction. Direct reduction of
femoral neck fractures are not routinely taught, nor practiced, clamp
application-placement, plating of the neck etc. So probably he underwent exposure
of the anterior-caudal portion of the neck with more indirect
manipulation-reduction prior to screw placement. I believe that a Watson
Jones approach
extension to the lateral approach should afford both direct and adequate
visualization of the the entire neck for bone grafting-ORIF. The osteotomy option
although still viable-could always be a later procedure as the injury angle
(pauwels) portends a osteotomy angle out of the norm.
Good Luck
Sam Agnew, MD, FACS
Arlington Heights, Illinois 60005
Professor-Orthopedic Surgery
Harborview Medical Center
Seattle, WA 98104-2499
Ural Scientific Research Institute of Traumatology and Orthopaedics
7, Bankovsky str. Ekaterinburg 620014 Russia
Director, Orthopaedic Trauma
Mcleod Regional Medical Center
Arlington Orthopedics and Hand Surgery Specialists, Ltd.
1100 W. Central Road, Suite 304
Arlington Heights, Illinois 60005
Orthopaedic Trauma
901 East Cheves St Suite 100
Florence, SC 29503