
Date: 04/04/00 09:30PM
Subject: Bilateral Pilon Fxs
From: Issa AbuRiziq
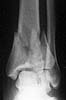
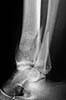
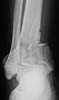
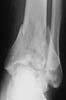
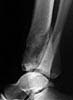
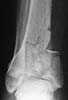
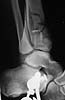
A 17 year old obese female (height 5.5 feet, weight 15 stones), sustained bilateral closed pilon fractures + vertical fracture left talus + tuberosity fracture of right os calcis. This occurred as a result of a fall from about three metres height, for a bet (a dare!).
Also has Right posterior tibial nerve neuropraxia and on admission had absent right dorsalis pedis pulse.
 |
 |
 |
 |
 |
 |
 |
 |
 |
 |
How would members of the list manage this?
Issa AbuRiziq - Locum Consultant Orthopaedic Surgeon at Monklands
Hospital - Airdrie - Scotland - UK.
Date: Tue, 04 Apr 2000 13:57:36 -0500
From: Adam Starr
I would fix them both.
Provided the soft tissues are in good shape, I would treat both pilon fx's, and the L sided talus fracture, with ORIF. Here at Parkland we use medial and lateral longitudinal incisions to approach pilon fxs, rather than an anterior "AO style" approach.
If the patient has open wounds or severely traumatized skin (abrasions or fracture blisters or significant swelling) then I would temporize with bilateral ankle-bridging ex-fix frames. Leave them on until the soft tissues improve.
There are plenty of people who feel strongly that definitive ex-fix with limited internal fixation (such as a couple perc screws) gives good results with far less complications.
However, I think the recent articles in the JOT (Sirkin et al., 13, pp 78-84, and Patterson and Cole, 13, pp 85-91) have shown an acceptable decrease in soft tissue problems using a technique of temporary ex-fix followed by ORIF.
I jumped on the ankle bridging ex-fix bandwagon as hard as anybody a couple years ago. My personal experience (warning! warning! BIAS ALERT) is that you'll see better results if you can achieve a better reduction. So now I tend to fix them...as long as the soft tissue is okay.
You know this is one of the most contentious areas in orthopaedic trauma. It'll be fun to read all the replies.
Good luck.
Adam Starr, Dallas
Date: Wed, 05 Apr 2000 21:00:42 +0800
From: efont
I have done single pilon fractures not bilateral, and from the experience i and my colleagues at the Armed forces have gathered from parachute jumping injuries, minimal internal fixation to reduce extensive soft tissue injury during surgery coupled with external fixation provides the best result ( less necrosis of skin) by using wires and screws for non-rigid fixation to achieve reduction. We rely on the ex fix to provide the rigid fixation. Some would try percutaneous multiple k-wire fixation and then ex-fix.
What i am worried about is the foot with negative dorsalis pedis pulse . I think it deserves further studies.
Date: Wed, 05 Apr 2000 15:13:34 -0500
From: Steven Rabin
A lot depends on the soft tissues. I usually start with a spanning external fixator at both sides to maintain length and watch for compartment syndrome of the foot and let the swelling subside. I then come back and either definitively fix with ORIF if i'm very sure that the skin is in good condition and especially if the patient is young and not a smoker or diabetic because i think the best long term results are with anatomic reduction.
It is very important to be honest with yourself about the soft tissue condition. It is no fun to see the plate without an x-ray when the patient returns to the clinic.
If the soft tissues are bad and don't seem to be getting better quickly, i might opt for limited internal fixation maintaining the fixator or adjusting it. J. Tracy Watson presented a nice (paper at last year's OTA meeting (and also at the ASAMI meeting) on the lack of deep infections when the fixator is prep'd into the surgery site without removing its individual parts or resterilizing them.
When the pieces are too small for reliabale internal fixation, the Ilizarov type frames are certainly useful here, but i have encountered poor patient compliance and tolerance with bilateral ring fixators.
Again i would emphasize that the soft tissues need to take precedence. Failure of fixation or malunion are relatively treatable conditions when the patient's leg can better tolerate surgery. (Bilateral ankle fusions would not be fun, but would be better than bilateral amputations from infected nonunions...) A staged procedure when the skin is better might avoid skin slough and free flaps.
I wouldn't use multiple k-wires. the fixation isn't rigid or stable enough to really help and wires can bend or break. If you can achieve adequate reduction to get the percutaneous k-wires in, then you might as well use guide pins instead of k-wires and immediately replace them with percutaneous cannulated screws.
Date: Wed, 12 Apr 2000 19:19:35 -0700
From: Issa AbuRiziq
This patient had ORIF of her left Pilon fracture.
 |
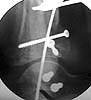 |
The Right ankle remains on skeletal traction.
Any views or comments/opinions from the members of the group?
Issa AbuRiziq - Locum Consultant Orthopaedic Surgeon at Monklands Hospital - Airdrie - Scotland - UK.
Date: Wed, 12 Apr 2000 15:10:19 -0500
From: Adam Starr
Was a medial ex-fix used to hold the tibia out to length? Is there a frame still in place?
Date: Wed, 12 Apr 2000 18:12:31 -0400
From: bruce meinhard
The goals are 1. fibular length which was achieved. 2. articular restoration which was incongruous at the medial side on the mortise view some additional help by way of pushing out the diepunch component and inserting (3.) bonegraft or its substitute would help. 4. medial butress which was not achieved and which could have been a subcutaneous plate or a medial ex fix.
If this is your definitive fixation and you intend to keep the patient supine until healing, DVT propyhlaxis should be therapeutic levels of coumadin. Do you plan casting and bed to wheel chair? still in this case, I would keep the INR 2-3X normal under these circumstances. A supplemental external fixator would allow more mobility. It could be placed medially with two pins into the calcaneus and two in the shaft of the tibia. Nice work so far.
BPM
Date: Thu, 13 Apr 2000 19:02:42 -0700
From: Issa Aburiziq
This patient is under the care of one of my colleagues here at Monklands.
A medial ex-fix was not used. There is no frame, but a B/K plaster cast.
I believe that the plan for the right ankle next week is to insert a transverse high tibial Denham (or Steinman) pin and incorporate both this pin and the os calcis Denham pin in a complete B/K plaster cast maintaining distraction and ligamentotaxis.
Any Opinions about this proposed method of treatment?
SC Enoxaparin is used routinely in our unit for DVT prophylaxis usually 20-40mg once daily.
Date: Thu, 13 Apr 2000 15:39:58 -0400
From: bruce meinhard
A plaster cast with pins incorporated is an external fixator without the ability to inspect the skin. If the skin is without lesions and without fear of breakdown then it should suffice for your intended purposes.
BPM
Date: Thu, 13 Apr 2000 15:53:27 -0500
From: Adam Starr
You're mixing cast immobilization and internal fixation with a bunch of K-wires. So, you get all the downside of surgery (scarring, dissection, possible infection) and none of the up-spide (early range of motion, anatomic stable fixation), PLUS you get the downside of cast treatment (stiffness and atrophy) with none of the upside (avoidance of surgery).
I wouldn't have done it this way.
Adam Starr, Dallas, Texas